Medical Billing Workflow: The End-to-End SOP (Full Cycle, Clean Claims, and Fewer Denials)
Executive Takeaway
Medical billing isn’t “billing work.” It’s a chain of handoffs. When owners aren’t assigned and gates aren’t enforced, defects travel downstream, turn into denials, and then A/R teams spend their time reworking upstream mistakes.
Evidence Snapshot
The revenue cycle spans from the patient’s initial encounter through final payment.
Prior authorization and pre-claim review differ mainly by timing, and timing errors create avoidable rework.
The revenue cycle in healthcare connects services rendered with how providers receive compensation.
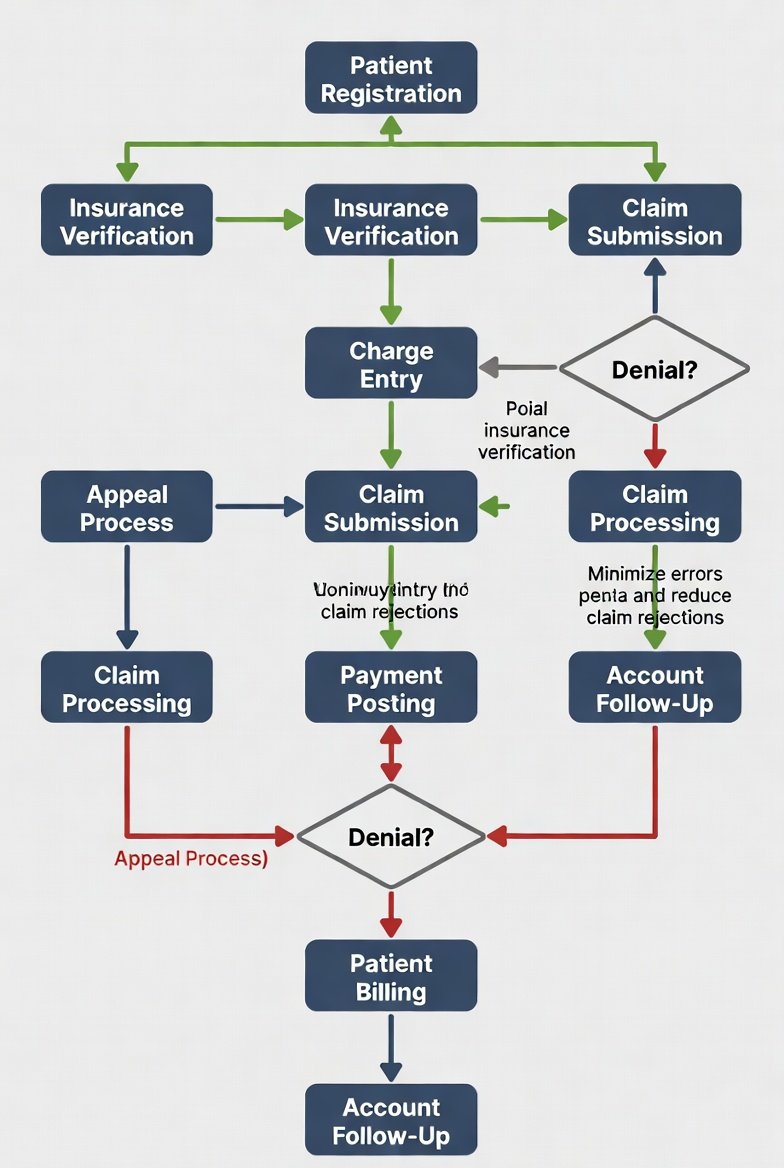
Workflow Diagram (Text Version)
Intake → Registration → Eligibility → Authorization / Medical Necessity → Encounter → Documentation → Coding / Charge Capture → Claim Build → Claim Edits / Scrub → Submission → Adjudication / ERA → Posting / Reconciliation → Denials / Appeals → A/R Follow-Up → Patient Balance → Final Payment / Close
If your team can’t say where a claim sits in this chain, you don’t have a workflow—you have people working tickets.
Who This SOP Is For
Best fit: multi-provider practices, specialty clinics, and hospitals/IDNs with enough volume that defects become a measurable tax.
Not ideal for: tiny cash-only clinics. They still need documentation, charge capture, and posting discipline, but not a fully role-separated SOP.
Role-by-Scale (How the Workflow Changes)
Scale | How Roles Usually Work | What Breaks If You Don’t Adjust |
Solo / Small Practice | One person wears multiple hats | Gates get skipped on busy days |
Group Practice | Access, coding, and billing are split | Handoffs fail without ownership |
Hospital / IDN | Specialized teams with governance | Visibility gaps slow close and lose work |
Operator line: bigger orgs don’t win because they’re bigger—they win because they enforce roles and gates consistently.
The Three-Zone Model (Fast Mental Map)
Front-End (Pre-Claim Gates)
Registration accuracy, eligibility verification, authorization timing and ownership, and financial clearance. This is where downstream chaos is prevented.
Mid-Cycle (Clinical + Coding Integrity)
Documentation completeness, coding quality, and charge capture discipline—where care becomes billable reality.
Back-End (Cash + Rework Loops)
Claim edits, submission, posting, denials, A/R follow-up, and patient balance resolution—where defects either resolve or compound.
Front-End Checklist (Ready-to-Bill Gate)
Registration complete with correct payer, plan, and identifiers.
Eligibility verified and documented (or exception logged).
Authorization status confirmed or documented not required.
Provider and location identifiers correct.
Patient responsibility expectations communicated.
Stop-the-line rule: if eligibility or authorization in medical billing is uncertain, do not push the claim through without a logged owner and exception.
Mid-Cycle Checklist (Coding-Ready Gate)
Documentation signed and complete.
Required elements present for the service type.
Charge capture complete with no missing services or supplies.
Coding supported by documentation.
Medical necessity support present where payer rules are strict.
Operator line: many “payer denials” are actually documentation or capture defects.
Back-End Checklist (Close-Ready Gate)
Claim edits resolved or approved by exception.
Submission accepted and tracked.
ERA/EOB posted accurately.
Allowed vs expected variances flagged.
Denials routed to reason-specific queues.
Repeat denial reasons logged and assigned upstream.
Patient balance resolution path defined.
Stop-the-line rule: unexplained variances do not get labeled “contractual” and ignored.
Medical Billing Workflow SOP (End-to-End Steps)
Intake and registration establish correct patient and insurance data.
Eligibility confirms active coverage.
Authorization and medical necessity workflows confirm payer requirements and ownership.
Financial clearance sets patient expectations.
The encounter occurs and care is delivered.
Documentation supports coding and necessity.
Coding and charge capture translate care into billable data.
Claims are built and scrubbed.
Claims are submitted and tracked.
Adjudication produces payment or denial outcomes.
Posting and reconciliation ensure accuracy and visibility.
Denials and appeals resolve issues and feed root causes upstream.
A/R follow-up manages aging balances.
Patient balances are resolved.
Final payment closes the cycle and revenue cycle management benefits.
HFMA defines the cycle through final payment—any SOP that stops earlier is incomplete.
Step → Metric Protected (SOP Guardrails)
Step | Metric It Protects | What You Watch |
Eligibility gate | Rejection rate | Rejections by reason |
Authorization ownership | Auth denial rate | “Missing auth” trend |
Documentation completion | Medical necessity denials | Denial mix |
Charge capture | Leakage | Charge lag, missing charges |
Claim edits | First-pass performance | Overrides and acceptance rate |
Posting QA | Underpayment leakage | Variance flags |
Denials root-cause | Repeat denials | Top repeat reasons |
Patient balance process | Cash predictability | Dispute rate and resolution time |
Top Failure Modes (What Actually Breaks)
Eligibility gets skipped on busy days.
Authorization isn’t clearly owned.
Documentation exists but doesn’t support necessity.
Charge capture lags behind care delivery.
Claim edits are overridden to push volume.
Posting variances are ignored.
Denial management in medical billing are worked but never closed upstream.
Each failure has the same fix: enforce the gate and assign ownership.
Operator Mini-Case
Mistake: claim edits were routinely overridden to keep volume moving.
Impact: rejections and denials rose, and staff time shifted to rework.
Fix: strict override policy plus weekly review of top overrides with owners assigned.
Outcome cue: within a month, overrides fell and first-pass acceptance improved (varies by specialty and payer mix).
Point of No Return (Workflow Version)
If the same defect appears twice, an upstream fix is required.
If an account receive able is aging with unresolved eligibility, authorization, or documentation issues, escalate immediately.
Do not let A/R teams carry upstream defects—that’s how cost-to-collect explodes quietly.
Fix In-House vs Outsource vs Software
Fix in-house first when gate skipping and ownership are the problem.
Outsource when backlogs and staffing gaps drive uncontrolled aging.
Software when visibility and routing are the bottleneck—but only after the SOP is enforced.
FAQs
What is the medical billing workflow?
It’s the end-to-end process from intake and eligibility through coding, claims submission, posting, denials and A/R follow-up, patient balance resolution, and final payment.
Why are claims rejected when coding is correct?
Because defects often occur earlier—registration, eligibility, authorization timing, or missing required fields.
What’s the fastest way to reduce denials without hiring?
Stop skipping gates, enforce edit policies, and require upstream fixes when defects repeat.
How do you improve efficiency without cutting corners?
Use owners, stop-the-line rules, and checklists. Efficiency comes from preventing defects, not pushing dirty volume.