Front-End Revenue Cycle: The Patient Access Process That Makes or Breaks Clean Claims
Executive Takeaway
Front-end revenue cycle isn’t “admin.” It’s your claim-quality engine. When patient access misses eligibility, authorization timing, or financial clearance, the back end turns into a rework loop—denials rise, A/R ages, and cash becomes unpredictable.
Evidence Snapshot
Prior authorization and pre-claim review differ mainly by timing and when services can begin—timing mistakes create preventable rework.
High insurance verification and clean-claim performance are commonly cited as claim-quality benchmarks (vary by specialty and payer mix).
Complete and accurate demographic and insurance information is tied to cleaner claims and stronger collections outcomes.
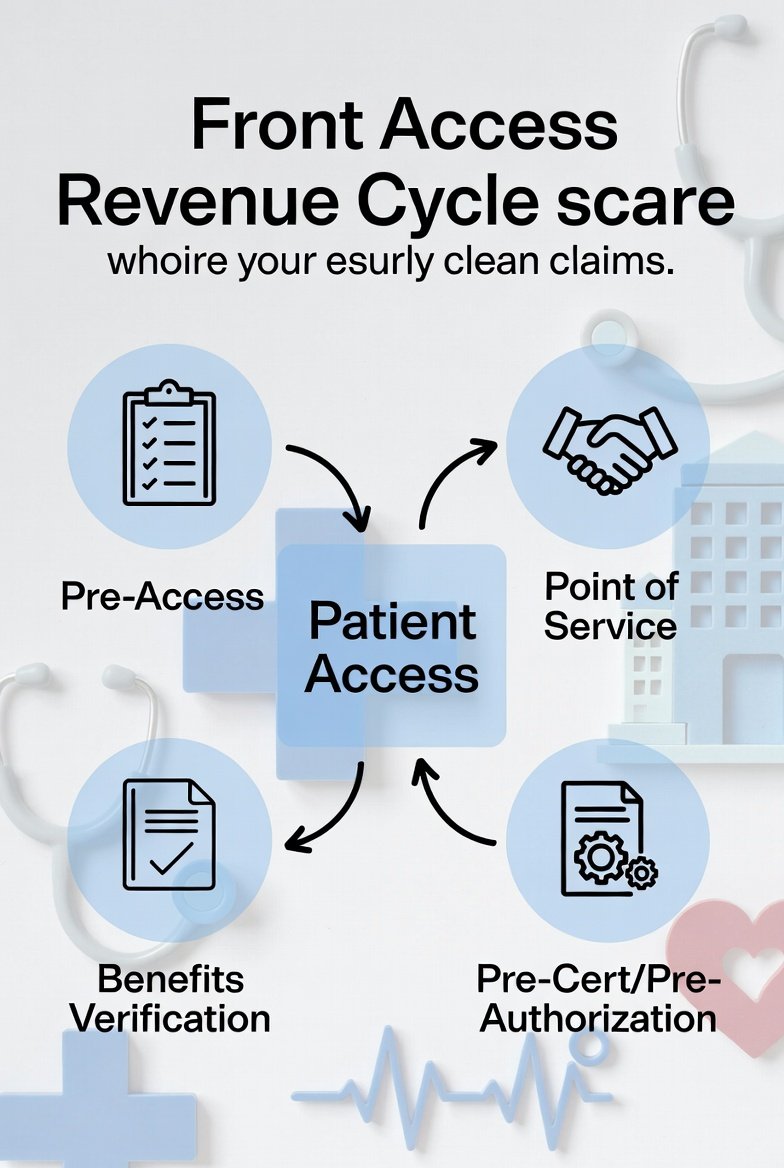
What “Front-End Revenue Cycle” Means (Plain English)
Front-end revenue cycle—often called patient access—is everything that happens before a claim is built:
Scheduling and pre-registration
Registration accuracy
Eligibility verification
Authorization and referral management
Financial clearance and estimates
Point-of-service collections
Clean handoff to coding and billing
Operator truth: most back-end problems are front-end defects that matured.
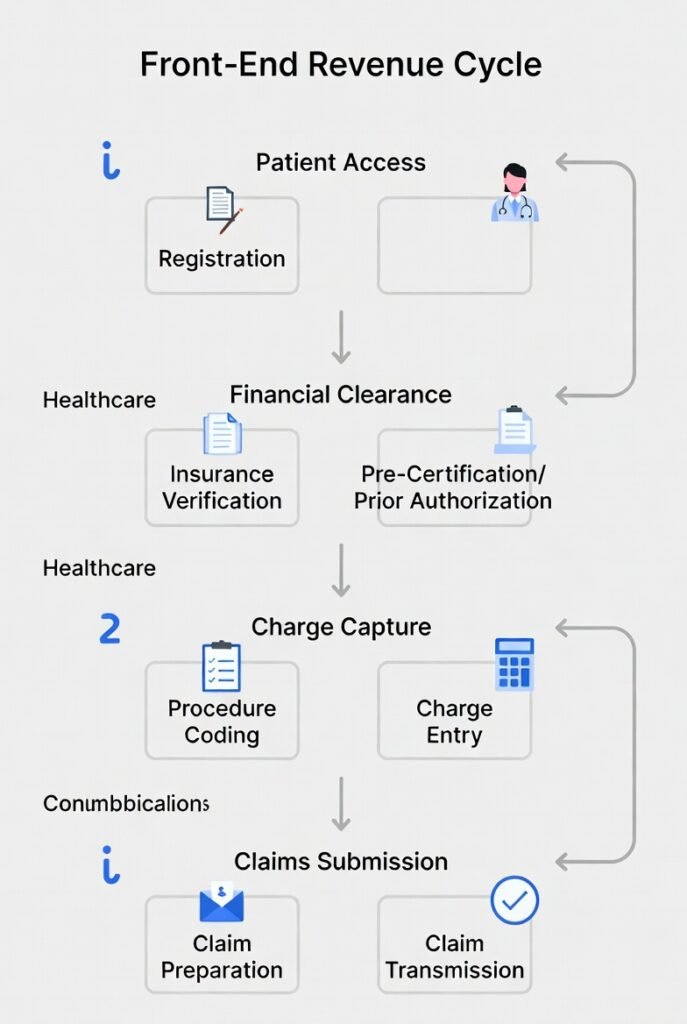
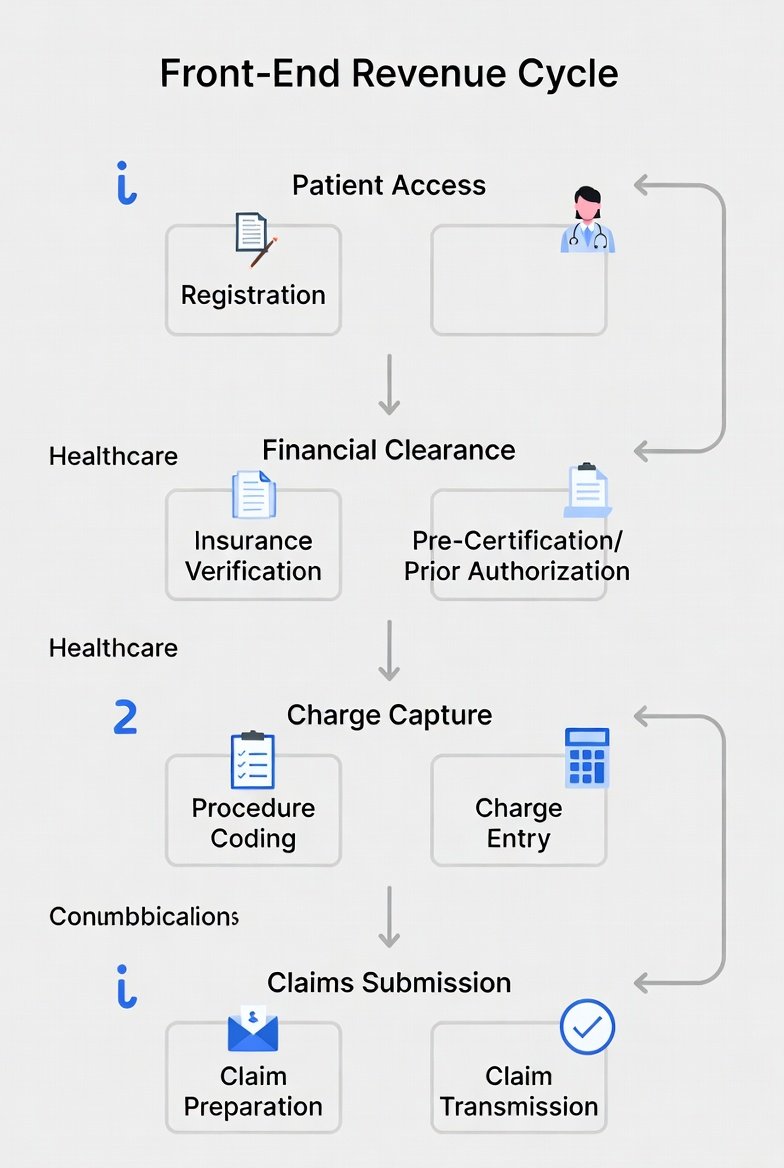
Front-End Revenue Cycle Flow
Scheduling → Pre-Registration → Registration → Eligibility → Authorization / Referrals → Financial Clearance / Estimates → POS Collections → Handoff Packet → Mid-Cycle (documentation and coding)
Who This Is For
Best for: multi-provider practices, specialty groups, hospitals, IDNs, and ASCs with payer rules and authorization complexity.
Not for: cash-only micro clinics. They still need registration and estimates, but full eligibility and authorization gates are minimal.
Front-End Revenue Cycle SOP (The Actual Process)
Step 1: Scheduling With Verification in Mind
Goal: capture enough information to verify coverage early.
Output: verification-ready appointment record.
Failure symptom: “we couldn’t verify because we didn’t have info.”
Step 2: Pre-Registration
Goal: reduce day-of errors and rushed data entry.
Output: pre-registration completed or flagged.
Failure symptom: check-in chaos and missing fields.
Step 3: Registration (Accuracy Gate)
Goal: correct demographics, payer sequence, plan identifiers, and subscriber data.
Output: clean registration file attached to the encounter.
Failure symptom: rejections due to mismatches or wrong payer.
Operator line: registration errors feel small until they cost weeks of delay.
Step 4: Eligibility Verification (Clean-Claim Gate)
Goal: confirm active coverage and service eligibility.
Output: eligibility verified with notes saved.
Stop-the-line rule:
If eligibility is unclear, log an owner, a reason, and a follow-up deadline. Otherwise, you’re pushing a denial downstream.
Step 5: Authorization and Referrals (Timing + Ownership)
Goal: determine if authorization or referral is required and who owns it.
Output: authorization number or documented “not required” basis.
Proof block (why timing matters):
Prior authorization decisions occur before services. Pre-claim review decisions occur before claim submission. Confusing the two creates denials that feel payer-driven but are actually workflow failures.
Stop-the-line rule: pending authorization without an owner is future denial churn.
Step 6: Financial Clearance (Set Expectations Early)
Goal: align the patient on expected responsibility and payment path.
Output: estimate acknowledgment and counseling path if needed.
Operator line: patient disputes are usually expectation failures, not patient failures.
Step 7: Point-of-Service Collections
Goal: collect known copays or balances respectfully and consistently.
Output: payment or defined next step (plan, assistance screening).
Failure symptom: avoidable patient A/R buildup.
Step 8: The Handoff Packet (Front-End → Mid-Cycle)
This is where weak workflows fail silently.
A complete handoff packet includes:
- eligibility result with timestamp
- authorization or referral status
- confirmed payer sequence
- financial notes (estimate, plan, assistance)
- verified patient contact details
- special medical billing flags (work comp, MVA, third party)
If billing chases front-end data, the workflow is broken by definition.
Front-End Checklists
Checklist A: Ready to Render Service
Pre-registration complete or flagged
Registration fields complete
Eligibility verified or exception logged
Authorization complete or pending with owner
Financial clearance path defined
Checklist B: Ready to Bill
Eligibility proof attached
Authorization status documented
Payer sequence confirmed
Patient responsibility documented
Handoff packet complete
Stage → Owner → Output → Failure Symptom
Stage | Owner | Output | Failure Symptom |
Scheduling | Scheduling | Verification-ready record | Missing info blocks verification |
Pre-registration | Patient access | Fields completed early | Rushed check-in errors |
Registration | Patient access | Clean payer and plan data | Mismatch rejections |
Eligibility | Patient access | Verified coverage proof | Preventable rejections |
Authorization | Auth / UR | Auth # or not-required doc | Missing-auth denials |
Financial clearance | PFS / counseling | Estimate or plan | Disputes, slow patient pay |
POS collections | Front desk / PFS | Payment or next step | Patient A/R growth |
Handoff packet | Access lead | Complete encounter packet | Billing chases info |
What Actually Breaks (Top Failure Modes)
Verification happens too late
Wrong payer sequence
Coverage terminated or mismatched
Authorization pending but service proceeds
Referral rules missed
Financial clearance skipped
POS collections inconsistent
No denial feedback loop to access
Handoff packet incomplete
Exceptions not tracked
Each failure has the same cure: enforce the gate and assign ownership.
Operator Mini-Case
Mistake: eligibility was inconsistent and authorization treated as “billing’s problem.”
Impact: preventable rejections and authorization denials delayed cash.
Fix: eligibility as a hard gate, auth ownership by service line, and mandatory handoff packet.
Outcome cue: within ~30 days, preventable rejects fell and billing stopped chasing front-end data (results vary by payer mix).
Point of No Return (Front-End Version)
Repeat defect twice in a week → fix the gate, not the account.
If an aging account still has unresolved eligibility or authorization issues, escalate immediately.
When A/R carries upstream defects, cost-to-collect explodes quietly.
Fix In-House vs Outsource vs Tools
Fix in-house when discipline and ownership are the issue.
Outsource when volume or staffing limits prevent timely verification and auth work.
Buy tools when visibility and routing are the bottleneck—but only after the SOP is enforced.
FAQs
What is the front-end revenue cycle in healthcare?
It’s the patient access portion of RCM—scheduling, registration, eligibility verification, authorizations and referrals, financial clearance, and POS collections before a claim is built.
Why do front-end errors cause denials and cash drag?
Eligibility and authorization timing mistakes create preventable rejections and denials that force late-stage rework.
What’s the fastest front-end fix for clean claims?
Treat eligibility as a gate, assign authorization ownership, and track exceptions with owners and deadlines.
How do you know the front end is working?
You’ll see fewer preventable rejections, fewer missing-auth denials, and more predictable first-pass performance.