Payment Posting in Medical Billing: Step-by-Step From Remittance to Reconciliation
Why Payment Posting Is a Control Function (Not Data Entry)
Payment posting is not just entering payments.
It’s how a remittance (ERA/EOB) and a deposit (EFT/check) become accurate balances, clean A/R visibility, and clear next actions.
When posting is sloppy, the damage is quiet:
- denials get buried
- underpayments go unnoticed
- “adjustments” become a hiding place for leakage
Operator goal: every deposit matched, every line posted correctly, every difference explained, every problem routed.
Evidence Snapshot (What’s Not Opinion)
- Medicare contractors send ERA using the HIPAA-standard X12 835 v5010.
- CAQH CORE Payment & Remittance operating rules define expectations around ERA/EFT workflows.
- ERA uses the X12 835 Health Care Claim Payment/Advice (005010X221A1) format.
Who This Is For
Small practices (1–10 providers)
You need a simple match deposit → post → route routine.
Large groups (10–100+ providers)
You need owned queues: posting vs variance vs denials.
Hospitals / IDNs
You need consistent posting rules across payers and tight reconciliation to prevent hidden leakage.
Not for: teams that expect posting staff to “fix everything” during posting.
Key Terms (Plain English)
- ERA: electronic explanation of how the payer processed claims.
- EOB: paper/portal version of the same info.
- EFT: the actual money deposit.
Translation: ERA explains why. EFT is the cash. Posting connects them.
What “Done” Looks Like
Payment posting is complete only when it is:
- Posted (payments and adjustments applied correctly)
- Routed (denials, underpayments, credits sent to queues)
- Reconciled (remittance, posting, and bank totals tie—or differences are owned)
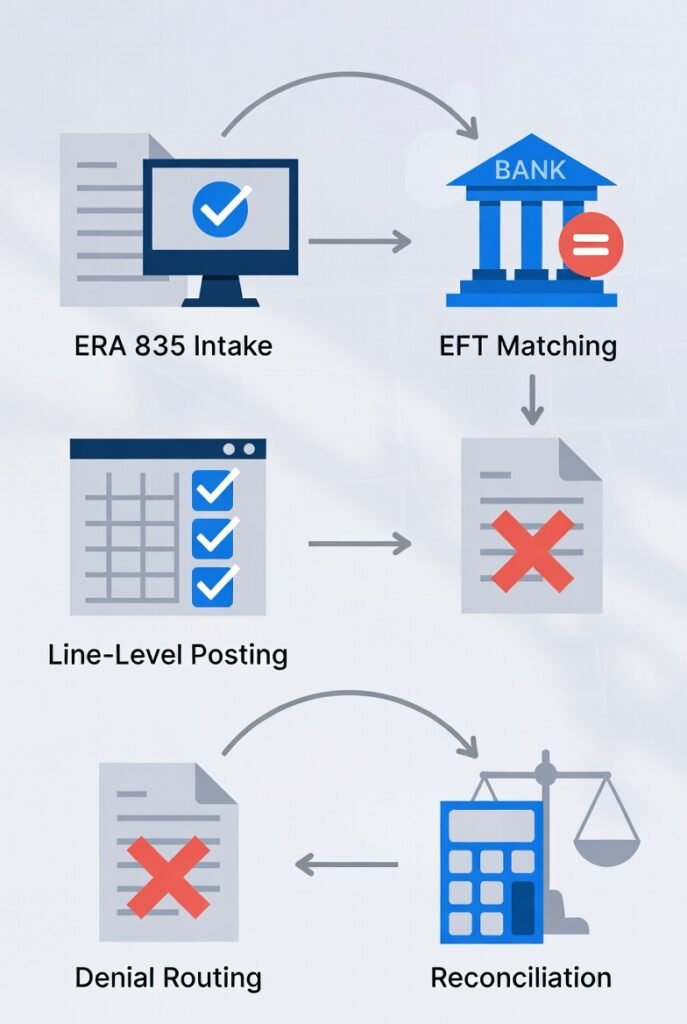
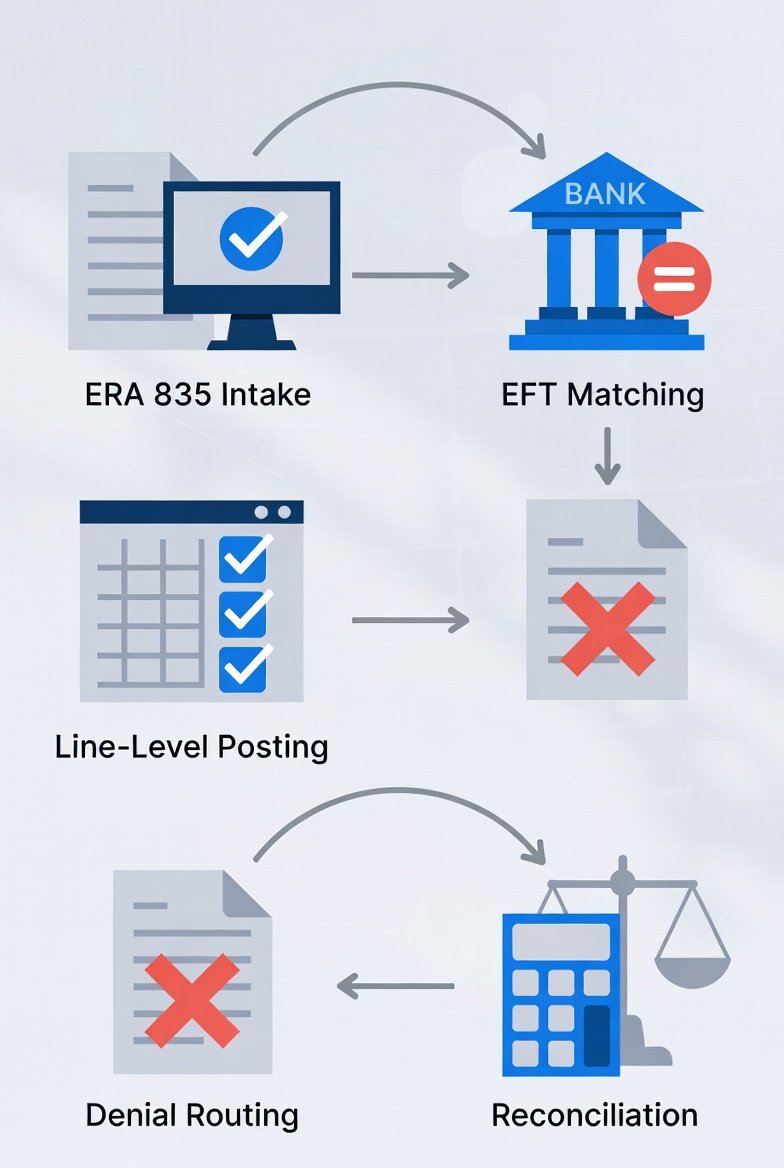
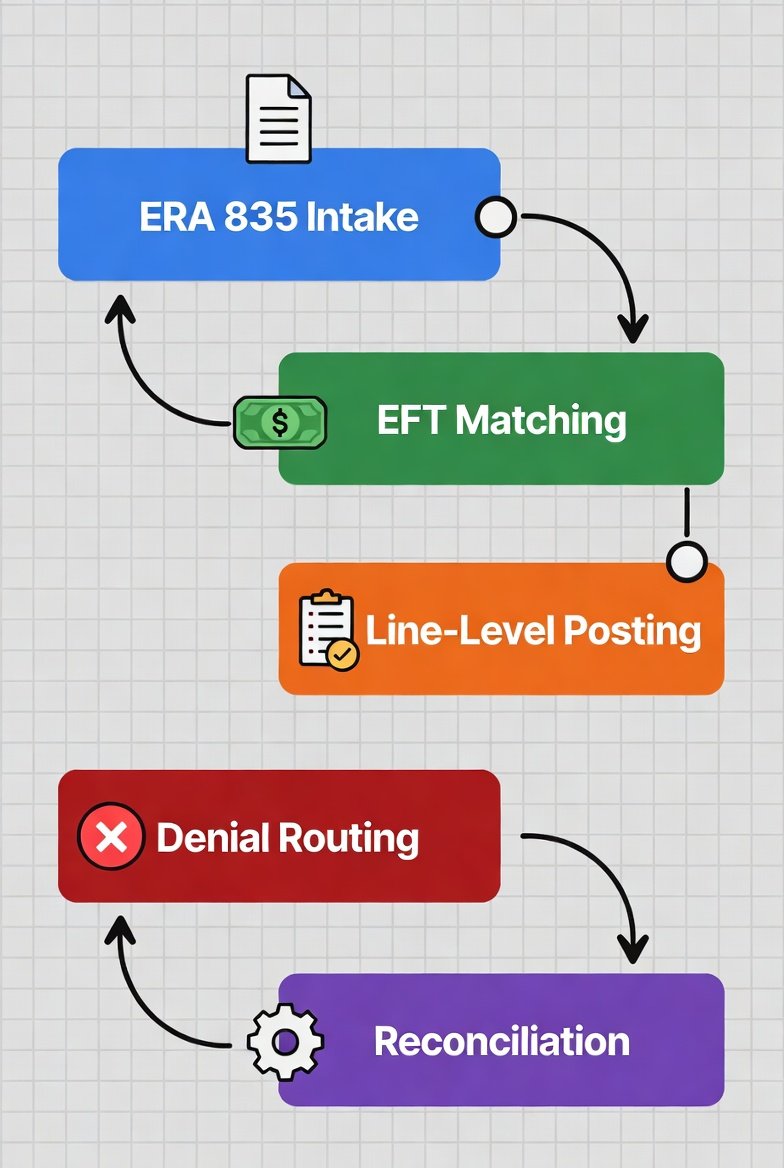
Step 1: Intake the Remittance (ERA/EOB Control)
Before posting anything, confirm followup:
- correct payer
- correct billing entity/NPI
- correct date range
- no duplicate import
- totals look reasonable versus expected deposits
Operator rule: no remittance is “ready” until it’s validated.
Step 2: Match the Deposit to the Remittance (Non-Negotiable Gate)
This is the control that prevents chaos.
Match rule:
- If EFT/check = remittance total paid → proceed
- If not → stop and identify why (offset, recoupment, split deposit, wrong file, duplicate)
Plain English: if cash and remittance don’t match, your ledger will lie.
Step 3: Post Payments at the Claim-Line Level
Line-level posting is where real issues show up.
Post at minimum:
- paid amount
- patient responsibility (if shown)
- adjustment with clear category
- denial indicator (if denied)
- allowed amount (if your system supports it)
Avoid lump-sum adjustments that erase meaning.
Step 4: Keep Adjustments Clean (So Losses Don’t Hide)
Use controlled categories:
- contractual (allowed vs charge)
- non-contractual (review required)
- takeback / recoupment
- correction / reversal
- small-balance write-off (policy-based)
Rule: if it reduces A/R, you must be able to explain it later.
Step 5: Post Denials as Denials (Then Route)
Never zero out denied lines just to “balance.”
Correct approach:
- post denial status clearly
- preserve denial reason
- route to denial work queue
That’s how denials get worked—and prevented.
Step 6: Identify Underpayments and Route Them
Underpayments hide because something was paid.
Triggers (examples):
- paid ≠ expected reimbursement
- repeat short-pays by payer or CPT
- known payer issues
Action:
- route to variance/underpayment queue
- assign owner + due date
- trend patterns weekly
Step 7: Reconcile Totals (Posting That Can Be Trusted)
Daily reconciliation (best practice):
- deposit totals = remittance totals
- posted payments = remittance “total paid”
- differences explained and owned
Weekly reconciliation = higher risk.
Plain English: posting without reconciliation is bookkeeping without a bank statement.
Step 8: Handle Credit Balances and Patient Payments
Credits balance are liabilities until resolved.
Minimum controls:
- weekly credit review
- refund/correction ownership
- correct application of patient payments
Posting Controls Table (Where Errors Surface)
Control Point | What You Verify | Owner | Failure Symptom |
Remittance intake | Correct ERA, no duplicate | Posting lead | Duplicate or wrong file posted |
Deposit match | EFT ties to ERA | Posting lead | Unapplied cash |
Line posting | Paid/adj/denial accurate | Posting team | Hidden denials |
Adjustment category | Correct bucket | Posting QA | Leakage buried |
Variance routing | Underpay/denial queued | Analyst | Silent loss |
Reconciliation | Totals tie | Billing lead | Month-end surprises |
Variance Types → Action Map
Variance Type | What It Signals | Route To | Risk If Ignored |
Denial | Coverage/policy issue | Denials queue | Write-off risk |
Underpayment | Short-pay | Variance queue | Revenue leakage |
Recoupment | Payer takeback | Reconciliation | Cash distortion |
Credit balance | Overpayment | Credit/refund queue | Compliance risk |
Unknown adj | Posting error | QA review | Reporting lies |
Mini Scenario
Mistake: posting staff use generic adjustments to zero balances.
Impact: denials and underpayments disappear into write-offs.
Fix: match EFT to ERA first, keep categories clean, route issues to owned queues.
Outcome cue: fewer month-end surprises and visible recoverable revenue.
Point of No Return
Posting mistakes get expensive after close—when statements go out and reversals trigger patient confusion.
Rule: reconcile and clear variances before close.
PASS / FAIL Checklist
PASS if
- ERA is correct and not duplicated
- EFT matches remittance (or exceptions owned)
- line-level posting with clean categories
- denials routed, not buried
- underpayments visible as a queue
- totals reconcile (or differences owned)
FAIL if
- posting happens without deposit match
- adjustments are a dumping ground
- denials disappear
- underpayments aren’t tracked
- reconciliation waits until month-end
By Practice Size
Small practice
One posting owner, one variance queue, simple checklist.
Large group
Separate posting vs variance vs denial roles; weekly trend review.
Hospital / IDN
Standardized rules, tight reconciliation, dedicated variance recovery.
30-Day Improvement Plan
Week 1: define “done” = posted + routed + reconciled
Week 2: enforce EFT-to-ERA match
Week 3: create denial, underpayment, credit queues
Week 4: review top patterns weekly and fix one upstream cause
Limitations
Offsets, recoupments, and payer behavior vary—but the discipline doesn’t:
match cash, keep categories clean, route issues, reconcile totals.