Revenue Cycle Process in Healthcare: The Full RCM Workflow (Steps, Owners, and What Breaks)
Executive Takeaway
Revenue cycle performance is driven by defect prevention upstream—every avoidable rejection, denial, or appeal creates cash drag and raises cost-to-collect.
The Revenue Cycle Process in One Sentence
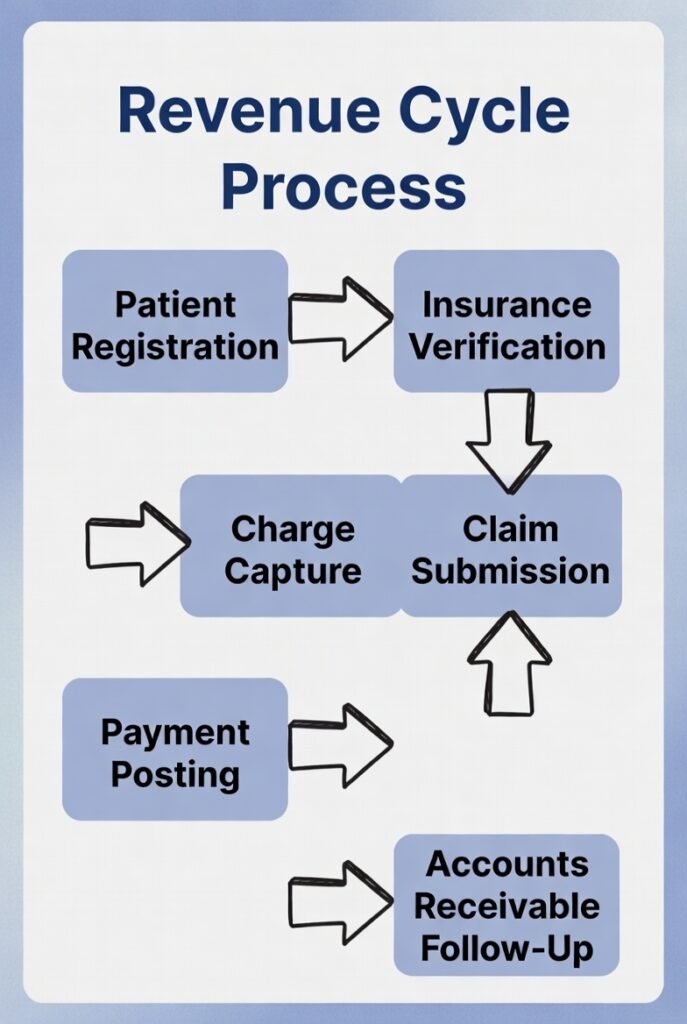
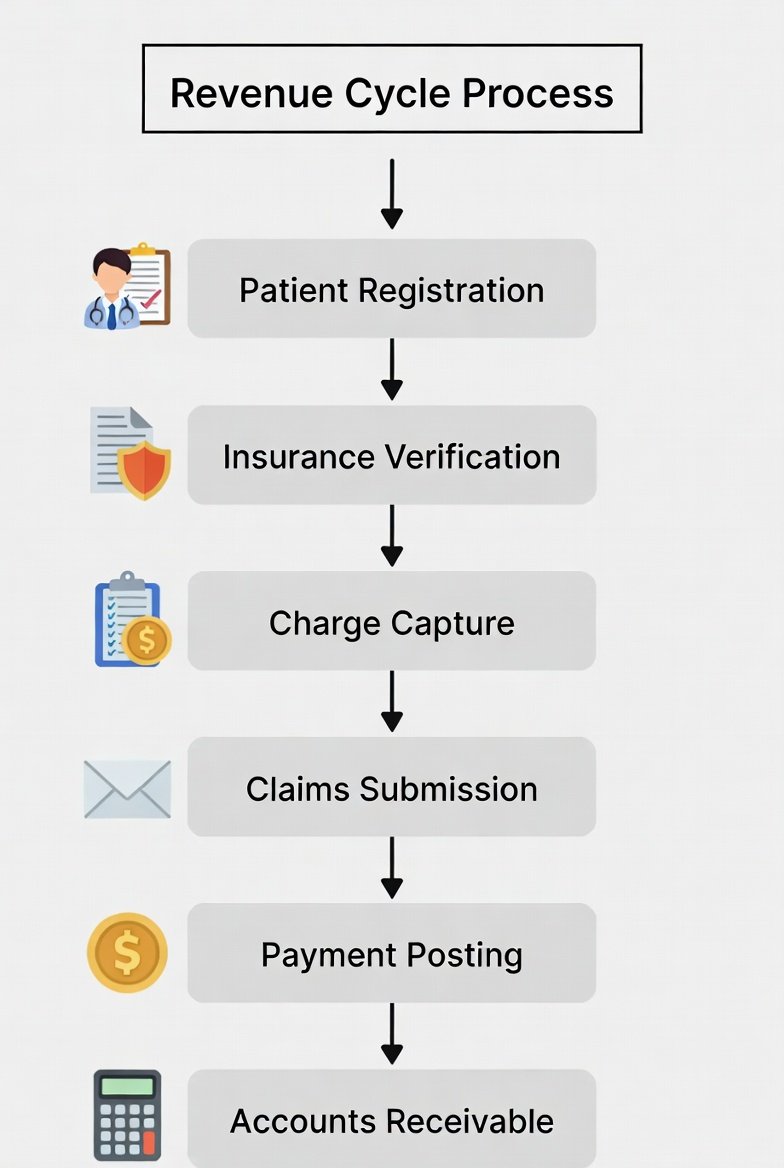
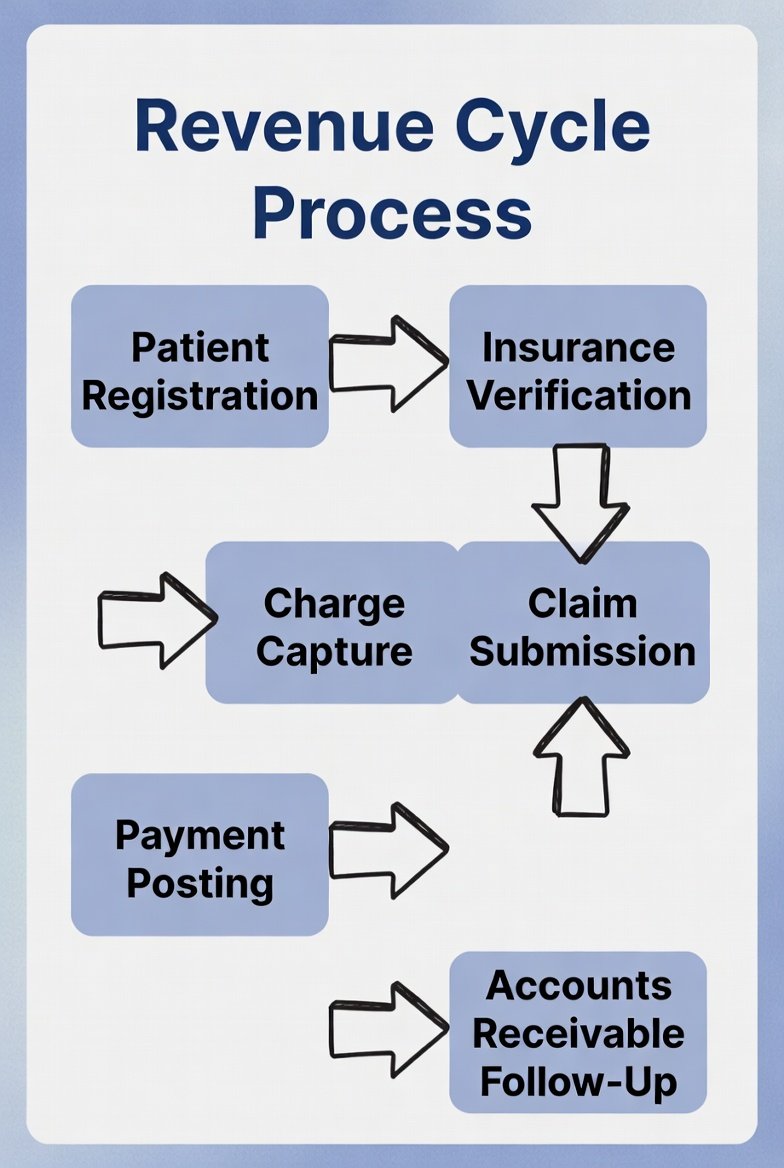
The revenue cycle process in healthcare is the end-to-end workflow that converts patient care into collected revenue—from first patient contact through eligibility and clearance, documentation and coding, claim submission, payment posting, denials resolution, and final patient balance resolution.
Who This Is For (And Who It’s Not)
This is for: hospitals and IDNs, multi-location physician groups, and established practices that run enough volume to require clear stage ownership and repeatable controls.
This is NOT for: solo or micro practices that don’t medical bill insurance or operate at a scale where formal RCM gates and role separation add value.
The Streamlined Revenue Cycle Workflow (10 Steps)
Revenue Cycle Workflow Table
Step # | Revenue Cycle Stage | What Happens |
1 | Scheduling & Pre-Registration | Capture basic demographics and insurance before the visit |
2 | Registration | Confirm identity, insurance, demographics, and signatures |
3 | Eligibility Verification | Verify active coverage and benefit rules |
4 | Authorization / Referral | Complete payer-required approvals |
5 | Financial Clearance & Estimate | Set patient responsibility expectations |
6 | Encounter & Documentation | Care delivered and documented |
7 | Coding & Charge Capture | Documentation translated into codes and charges |
8 | Claim Creation & Claim Edits | Claims built and scrubbed for errors |
9 | Submission & Payment Posting | Claims submitted, payments posted accurately |
10 | Denials, A/R & Patient Balance | Resolve denials, follow up A/R, close balances |
Revenue Cycle Components (Simple)
RCM operates across three connected components:
Front-End:
Registration, eligibility, authorization, and patient estimates. The goal is to prevent avoidable denials and reduce patient confusion.
Mid-Cycle:
Documentation quality, coding accuracy, charge capture, and claim-quality gates. This is where claim integrity is protected.
Back-End:
Payment posting, denials and appeals, A/R follow-up, and patient collections. This is where cash is ultimately retrieved.
Ownership Table (Stage → Owner → Failure Symptom)
Stage | Typical Owner | Failure Symptom |
Pre-Registration / Scheduling | Scheduling Team | Missing info, wrong insurance captured |
Registration | Patient Access / Front Desk | Claim rejections, demographic mismatches |
Eligibility Verification | Clearance / Patient Access | Coverage denials, patient disputes |
Authorization / Referral | Authorization / UR Team | “Missing auth” denials, care delays |
Financial Estimates | Financial Counseling | Surprise balances, low patient pay |
Clinical Documentation | Providers / CDI Team | Medical necessity denials |
Coding & Charge Capture | Coding / Charge Integrity | Underbilling, late charges |
Claim Edits & Scrubbing | Billing Office | Dirty claims escaping quality gates |
Payment Posting & Reconciliation | Posting Team | Incorrect balances or adjustments |
Denials & A/R Follow-Up | Denials & A/R Team | Repeat denial reasons, A/R aging growth |
Key takeaway:
If everyone “shares” ownership, defects repeat.
The Rework Loop (Why Cost-to-Collect Rises)
When claims bounce, labor costs compound:
Reject → Resubmit → Deny → Appeal → Resubmit → Partial Pay → Rework Again
Point-of-No-Return Rule
If the same preventable failure reason occurs twice, stop reworking the claim and fix the upstream defect.
This rule forces the organization to learn instead of just working harder—and it sharply reduces denial churn.
Fix In-House vs Outsource vs Buy RCM Software
Fix in-house when the problem is discipline and ownership, not tools. Gates exist but aren’t enforced, and leadership can run weekly defect reviews.
Outsource when staffing gaps or turnover have created denial or A/R backlogs and fast capacity with reporting is needed.
Buy or upgrade software when visibility and coordination pick up the most friction—weak denial analytics, weak work queues, or manual tracking.
Hard truth:
If you can’t see your top denial reasons weekly, you don’t have an RCM performance problem—you have a visibility problem.
Operator Mini-Case
A multi-location practice experienced denials that “felt random.”
Mistake: eligibility checks weren’t consistent; staff skipped verification on busy days.
Impact: rejections increased, rework volume climbed, and A/R began aging.
Fix: a hard gate was added—no encounter could close without eligibility status recorded (or a documented exception). Weekly reviews focused on the top three rejection reasons.
Outcome cue: rejections dropped within 30 days and rework became predictable (results vary by payer mix and baseline).
KPIs to Watch by Stage
Front-end KPIs: eligibility verified rate, authorization turnaround time, estimate completion rate.
Mid-cycle KPIs: coding edit rate, charge lag, claim edit override rate.
Back-end KPIs: denial rate by reason, days in A/R, percentage of A/R over 90 days.
Pick the KPI that reflects upstream defect creation—that’s where leverage lives.
FAQs
What breaks first when the revenue cycle slows down?
Usually eligibility discipline, authorization ownership, or charge capture and claim-edit enforcement.
Why do denials keep repeating after we work them?
Because the upstream defect wasn’t fixed. Track top denial reasons weekly and install a gate.
Is prior authorization part of the revenue cycle process?
Yes. CMS explains prior authorization and pre-claim review differ mainly by timing and when services can begin.
What are the components of revenue cycle management?
Front-end patient access, mid-cycle integrity work (documentation, coding, charge capture), and back-end cash retrieval (posting, denials, A/R).