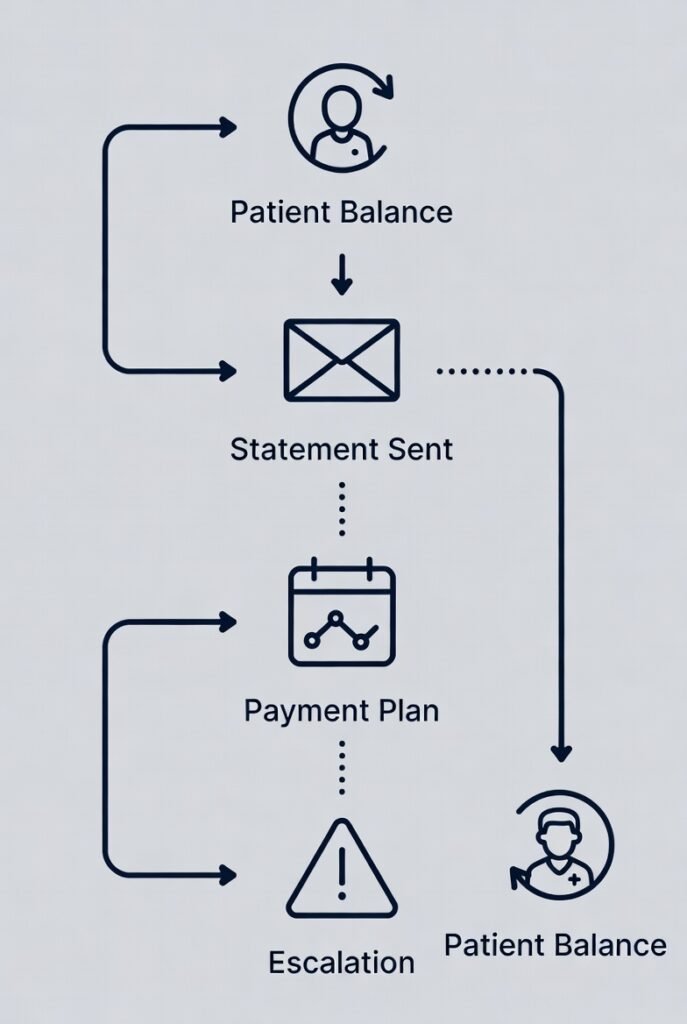
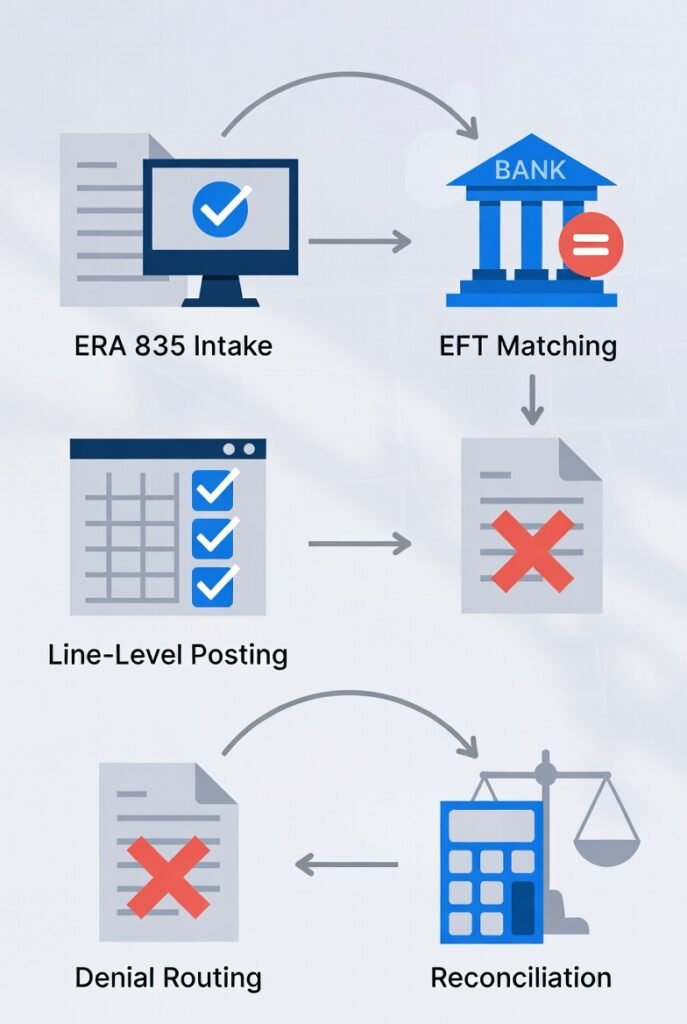
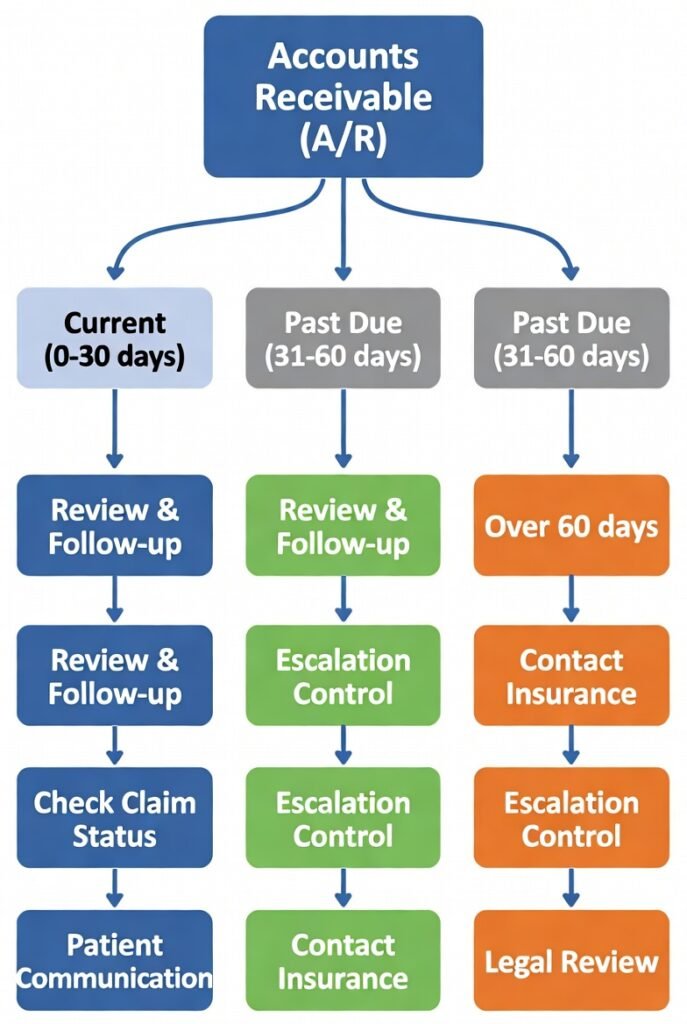
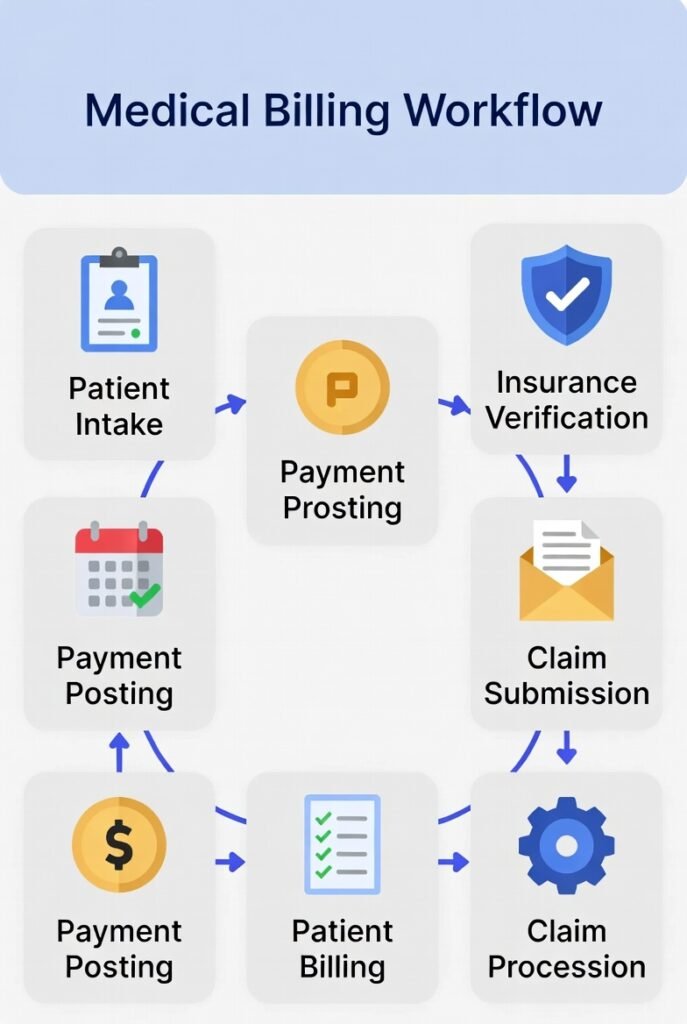
Collections in Medical Billing: Patient Balance Workflow, Payment Plans, and a Clean Escalation Timeline
Collections in Medical Billing: A Practical Collections Playbook Why Collections Is Account Resolution (Not Pressure) Collections in medical billing is account resolution, not pressure. The job is to move patient balances to a clear end state:paid, on plan, adjusted correctly, or documented and closed—without confusing bills, random follow-up, or inconsistent escalation. Most pages talk about […]