Collections in Medical Billing: A Practical Collections Playbook
Why Collections Is Account Resolution (Not Pressure)
Collections in medical billing is account resolution, not pressure.
The job is to move patient balances to a clear end state:
paid, on plan, adjusted correctly, or documented and closed—without confusing bills, random follow-up, or inconsistent escalation.
Most pages talk about POS collections and payment plans.
What actually improves cash and reduces disputes is execution discipline:
- a pre-statement accuracy gate
- a clean split between insurance vs patient responsibility
- a simple dispute workflow
- a predictable timeline patients can understand
This playbook is built to run in real billing management operations.
Evidence Snapshot (What’s Not Opinion)
- HFMA best practices emphasize clarity, consistency, and transparency in patient financial communications.
- CMS guidance limits when providers may request prepayment for Medicare deductible/coinsurance and ties it to routine/customary practice.
- CAQH CORE Claim submission Status (276/277) Infrastructure Rule includes real-time response expectations (~20 seconds) and availability targets (~86%) for CORE-certified entities.
Who This Is For
Small practices (1–10 providers)
You need a simple routine so patient balances don’t get forgotten.
Large groups (10–100+ providers)
You need role clarity: statements vs disputes vs plans.
Hospitals / IDNs
You need standardized communications, assistance routing, and consistent escalation.
Not for: teams that bill first and explain later.
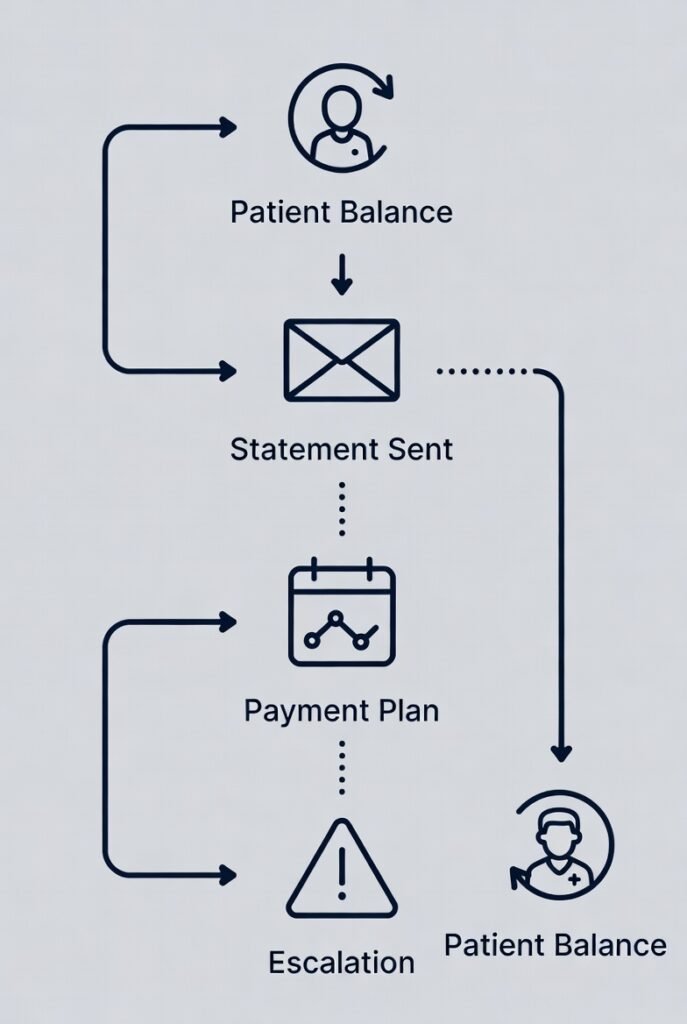
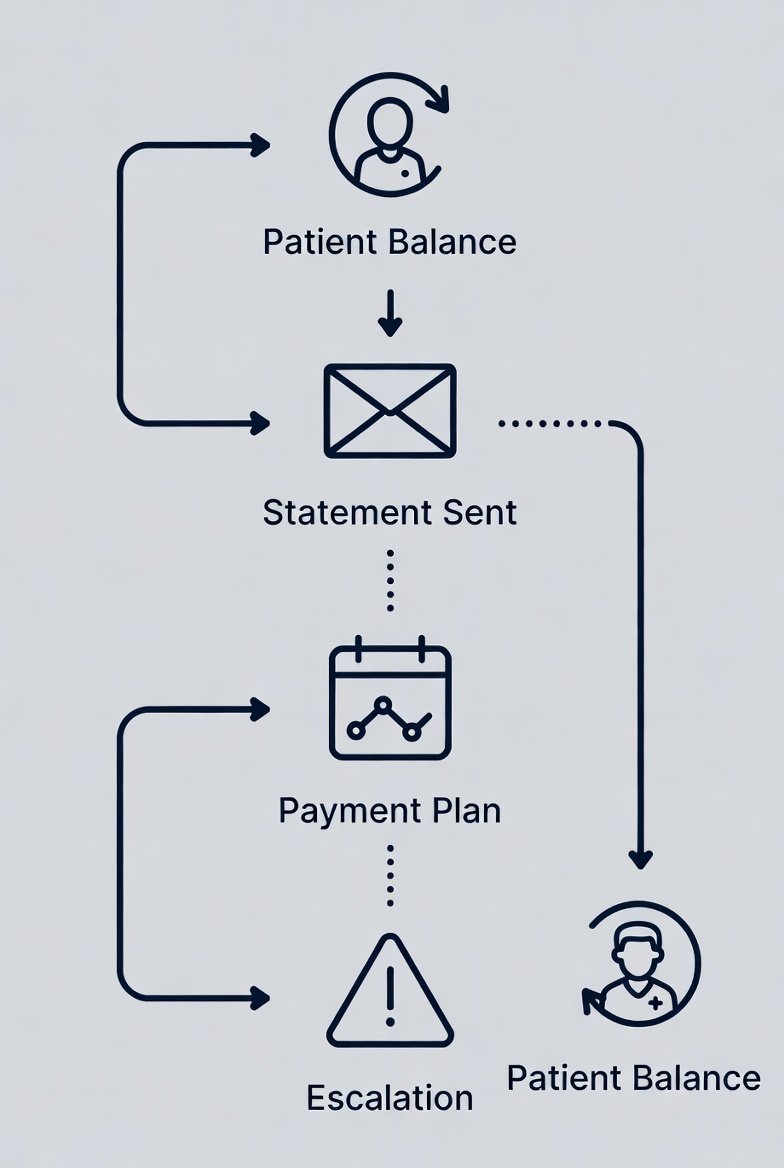
What Collections Includes (End-to-End)
Collections covers the full cycle of resolving patient balances:
- front-end prevention and expectations
- point-of-service collections (when appropriate)
- clear statements
- disputes and corrections
- payment posting plans
- assistance routing (per policy)
- escalation and close-out
Plain English: if the bill isn’t understandable, patients don’t pay faster—they delay or dispute.
Step 1: Run a Pre-Statement Accuracy Gate (Most Missed Control)
Before the first statement goes out, confirm the balance is real.
A large share of “patient A/R” is actually insurance or posting work in disguise.
Pre-Statement Accuracy Gate (Must-Pass)
Check | What You Confirm | If It Fails |
Insurance status | Adjudicated or documented patient responsibility | Route back to insurance follow-up |
Posting accuracy | Payments & adjustments categorized correctly | Correct posting before billing |
Responsibility type | Copay / coinsurance / deductible clearly identified | Clarify before statement |
COB validation | Correct payer order applied | Fix COB first |
Contact info | Address + phone/email verified | Update before billing |
Rule: don’t bill patients for balances that belong in insurance follow-up.
Step 2: Set Expectations Early (Collections Starts Before the Visit)
If patients learn about responsibility only after the visit, disputes rise.
Front-end actions that reduce collections friction:
- confirm demographics and contact preferences
- confirm coverage where available
- explain deductible/coinsurance in one sentence
CMS note: Medicare prepayment requests are limited and must follow routine/customary practice for similar non-Medicare patients.
Step 3: Use Patient-Friendly Financial Communication
HFMA emphasizes clarity and transparency.
A good statement must:
- show one clear balance due
- explain why (DOS + payer action + responsibility type)
- give 2–3 easy ways to pay
- offer one calm path for questions
Plain English: if your statement reads like a denial code sheet, you’re creating disputes.
Step 4: Make Paying Easier Than Avoiding
Collections improve when friction is low.
High-impact options:
- online portal payment
- text-to-pay (if allowed)
- card-on-file (with consent)
- autopay for plans
- plan setup in under 3 minutes
Rule: reduce friction before reducing price.
Step 5: Payment Plans That Actually Resolve Accounts
Plans fail when:
- the first payment isn’t collected
- terms are unclear
- plans are so long they become invisible
Plan basics that work:
- first payment at enrollment (when possible)
- clear cadence and end date
- simple reminders
- easy change path if the patient calls early
Step 6: Dispute Workflow (Calm, Fast, Repeatable)
Most disputes are confusion, not fraud.
What patients usually mean:
- “I don’t recognize this charge.”
- “Insurance should pay more.”
- “I expected a different price.”
Dispute flow:
- verify identity + DOS
- provide itemization/summary per policy
- check insurance status
- route appropriately:
- insurance pending → insurance lane
- denial → correction/appeal lane
- true patient responsibility → explain + offer options
Plain English: patients aren’t difficult—they’re uncertain.
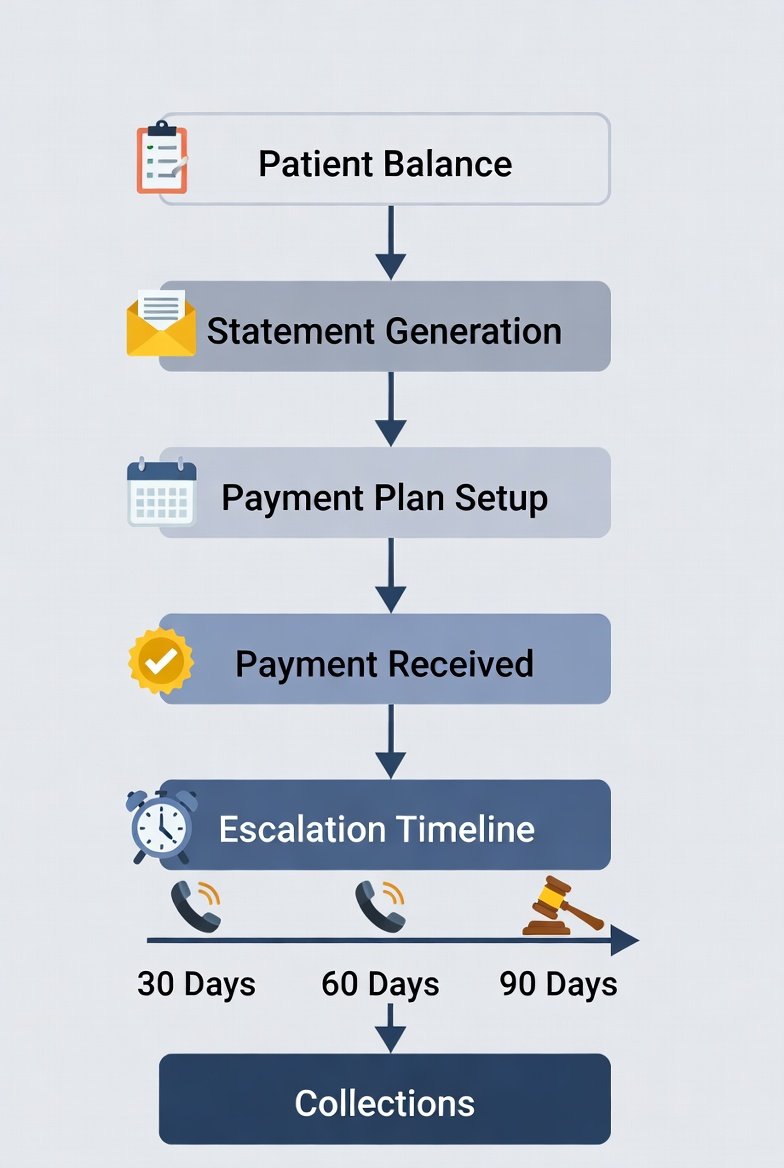
Step 7: Use a Predictable Escalation Timeline
Patients respond better when the process is predictable and consistent.
Patient Collections Resolution Timeline
Day Range | What the Patient Sees | What Billing Does |
Day 0 | Balance becomes patient responsibility | Confirm posting + responsibility |
Day 1–3 | Statement 1 | Clear explanation + pay options |
Day 10–14 | Reminder | Offer payment plan |
Day 20–30 | Statement 2 | “Let’s resolve this” messaging |
Day 35–45 | Final notice | Last plan/assistance review |
Day 60+ | Escalation review | Next step per policy |
Rule: escalation is policy-driven, not mood-driven.
Mini Scenario
Mistake: statements sent while insurance is unresolved and explanation is unclear.
Impact: angry calls, rework, balances age.
Fix: pre-statement gate + insurance/patient split + clear statements.
Outcome: fewer disputes, fewer calls, faster resolution.
PASS / FAIL Before Escalation
PASS if
- balance is confirmed (not pending insurance)
- statement explains the balance clearly
- dispute path was offered and documented
- payment plan option was offered when appropriate
- assistance routing was considered
FAIL if
- insurance outcome is unclear
- posting may be wrong
- patient never received a clear explanation
- an active dispute exists
- no workable payment path was offered
Collections by Scale
Small practice
Simple statements, 2 pay options, short plan flow.
Large group
Separate roles, standard scripts, consistent policy.
Hospital / IDN
HFMA-aligned communications, assistance routing, resolution metrics.
Hidden Costs of Bad Collections
- rework from insurance/posting confusion
- patient dissatisfaction
- staff burnout
- write-offs due to lost context
Measure resolved accounts per cycle—not calls per day.
Limitations
Patient responsibility and assistance rules vary by payer and policy.
What doesn’t vary:
confirm the balance → communicate