Revenue Cycle Middle Office: The Mid-Cycle Handoffs Hub (What It Is, Who Owns It, What Breaks)
Executive Takeaway
The middle office is where care delivered becomes claim-ready. If documentation-ready, coding-ready, and claim-ready gates aren’t enforced, the back end inherits defects and turns into a denial-and-rework factory.
Evidence Snapshot
Revenue cycle includes the administrative and clinical functions required to capture, manage, and collect patient service revenue.
Mid revenue cycle sits between patient access and business office functions.
Mid-cycle aggregates clinical and financial information to support clinical review and streamline coding and billing workflows.
What “Revenue Cycle Middle Office” Actually Means
In most organizations, the middle office maps to mid-cycle operations—the functions that sit between:
Front end / patient access (registration, eligibility, authorization)
and
Back end / business office (claim submission, posting, denials, A/R)
ICD10monitor explicitly places mid-cycle between patient access and the business office. That’s the cleanest definition to publish.
Plain English: middle office is the handoff engine that prevents clinical and administrative defects from turning into denials and leakage.
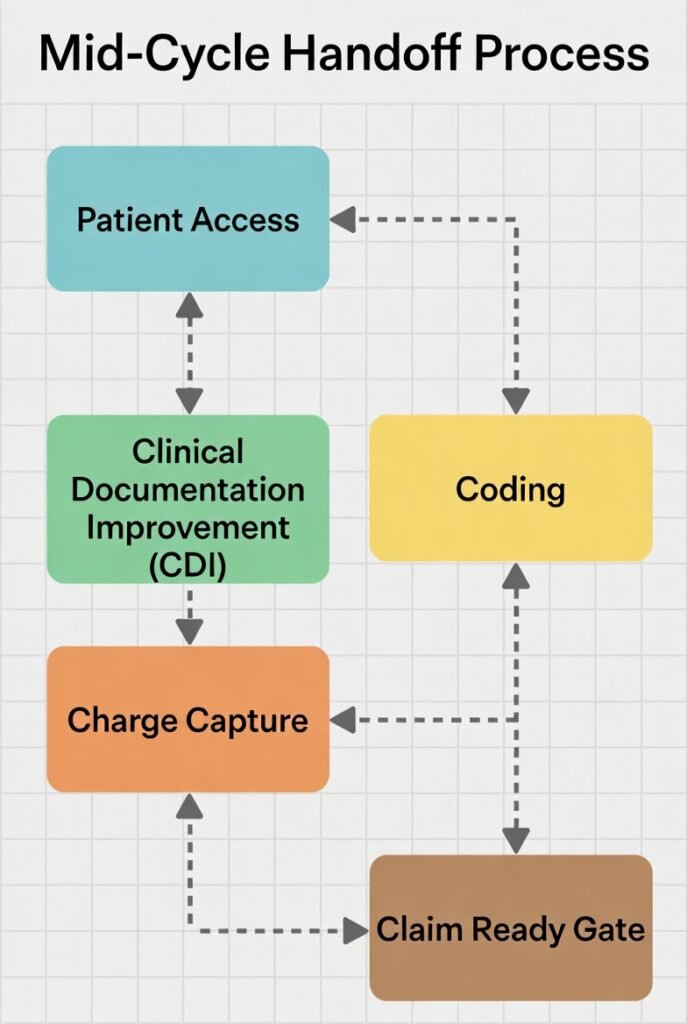
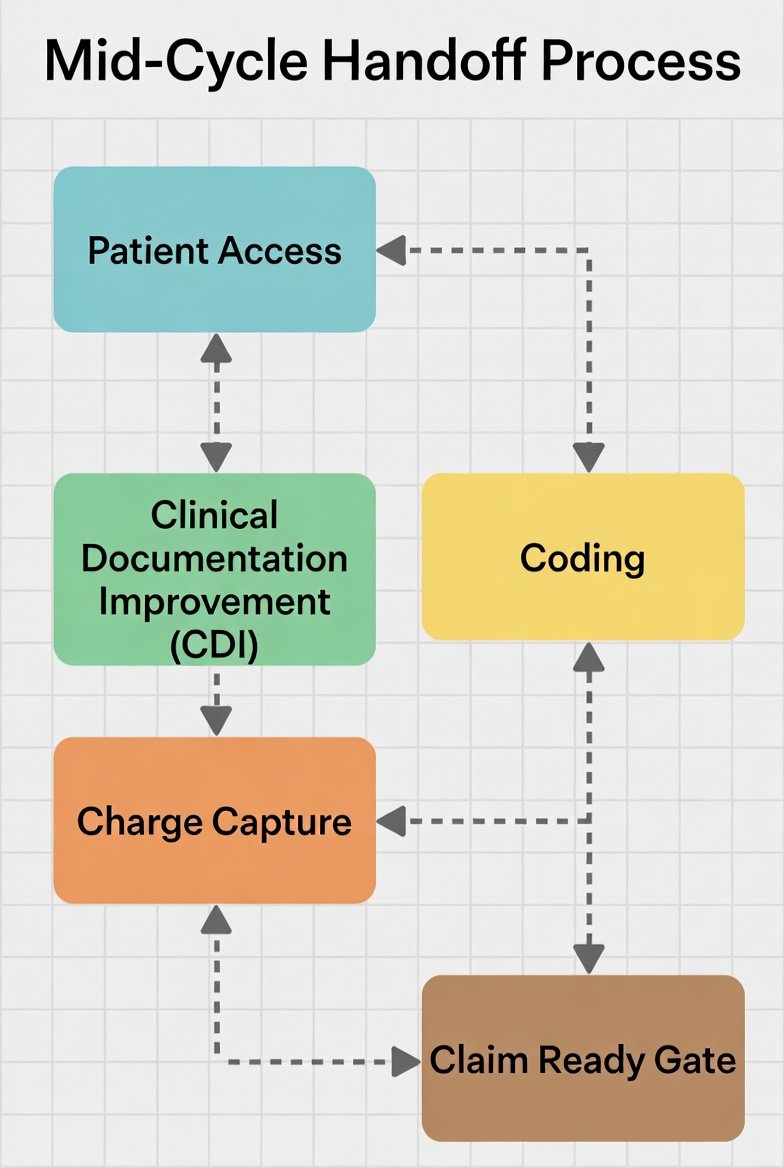
Middle Office Flow (Text Diagram)
Front End (verified patient, payer, authorization) →
Middle Office (documentation / CDI → coding → charge capture → HIM integrity → claim-ready gate) →
Back End (submission, posting, denials, A/R)
Who This Page Is For
Best for: hospitals, IDNs, ASCs, specialty groups, and multi-provider practices with coding volume and payer scrutiny.
Not for: cash-only micro practices. You still need documentation discipline, but the full mid-cycle stack is usually lighter.
Role-by-Scale (How Middle Office Looks in Reality)
Scale | Common Middle Office Setup | Risk If You Skip Structure |
Small practice | Provider + coder collaboration | Coding starts on incomplete notes |
Group practice | Coding team + light CDI/QA | Repeat denials never close upstream |
Hospital / IDN | CDI + coding + HIM + rev integrity | “Claim-ready” is assumed, not verified |
Operator line: volume doesn’t create mid-cycle—payer pressure does.
The Middle Office SOP (The 5 Pillars)
Pillar 1: Documentation Quality (CDI)
Goal: documentation supports what happened and why (medical billing necessity, specificity, completeness).
Failure symptom: medical-necessity denials, delayed coding, repeated queries.
Pillar 2: Coding Integrity (Accuracy + Consistency)
Goal: translate documentation into correct codes, modifiers, and settings.
Failure symptom: edits, denials, reimbursement instability, compliance risk.
Pillar 3: Charge Capture (Completeness + Timing)
Goal: bill everything performed—no leakage, no delay.
Failure symptom: missing charges, lagged charges, “we did it but didn’t bill it.”
Pillar 4: HIM / Record Integrity
Goal: audit-ready, retrievable records for payer requests and appeals.
Failure symptom: delayed appeals, missing documentation, slow payer response.
Pillar 5: Claim-Ready Gate
Goal: produce a reliable claim-ready signal.
Stop-the-line rule: if documentation, coding, or charge capture is incomplete → claim-ready = NO.
The Handoff Packets (Elite Tier)
Front End → Middle Office
Eligibility proof + timestamp
Authorization or referral status
Confirmed payer sequence
Patient identifiers validated
Financial clearance notes
Encounter attributes affecting coding
Middle Office → Back End
Documentation-ready status
Coding-ready status
Charge capture status
High-risk payer or necessity flags
Claim-ready yes/no with reason
Exceptions with owner and deadline
The middle office’s real product is clean handoffs.
Middle Office Checklists
Documentation-ready: note signed, required elements present, necessity supported, CDI queries tracked.
Coding-ready: documentation passed, codes supported, modifiers verified, QA completed if needed.
Claim-ready: coding complete, charges complete, exceptions logged, handoff attached.
Stage → Owner → Output → Failure Symptom
Stage | Owner | Output | Failure Symptom |
CDI | CDI lead / clinical | Complete notes | Necessity denials |
Coding | Coding manager | Coded encounter | Edits and denials |
Charge capture | Rev integrity | Complete charges | Leakage and lag |
HIM integrity | HIM lead | Audit-ready record | Slow appeals |
Claim-ready gate | Mid-cycle owner | Yes / No decision | Dirty claims downstream |
Step → Metric Protected (No Fake Numbers)
Gate | Metric Protected | What You Track |
Documentation-ready | Necessity denials | Query aging, denial mix |
Coding-ready | Edit failure | Edits by type, QA findings |
Charge capture | Leakage | Charge lag, missing charges |
HIM integrity | Appeal cycle time | Missing-doc rate |
Claim-ready signal | Clean claims | % claim-ready at submission |
Top Failure Modes (What Actually Breaks Mid-Cycle)
Coding begins before documentation is complete.
CDI is reactive instead of targeted.
Charge lag isn’t tracked.
Front-end auth/eligibility never reaches coding.
QA sampling is skipped.
Under payments posting hide inside “adjustments.”
Appeals happen without upstream fixes.
HIM retrieval is slow.
Claim-ready is assumed.
No single mid-cycle owner exists.
Each failure has the same fix: enforce the gate and assign ownership.
Operator Mini-Case
Mistake: documentation gaps were treated as minor; coding proceeded and charge lag wasn’t visible.
Impact: dirty claims rose, denials increased, staff time shifted to rework.
Fix: documentation-ready and claim-ready gates enforced; charge-lag queue added; handoff packets required.
Outcome cue: within ~30 days, avoidable rework dropped and claims went out cleaner (results vary by service line and payer mix).
Point of No Return (Mid-Cycle Version)
If documentation queries remain open past the deadline, claim-ready stays NO.
If a denial management reason repeats twice, change the upstream gate.
Never let the back end absorb mid-cycle defects—that’s how margin disappears quietly.
Fix In-House vs Outsource vs Buy Tools
Fix in-house when ownership and gate discipline are weak.
Outsource when chronic backlogs exceed internal capacity.
Buy tools when routing and visibility are the bottleneck—tools amplify gates, they don’t replace them.
FAQs
What is the revenue cycle middle office?
It’s the mid-cycle phase between patient access and the business office where documentation, coding, and charge capture determine claim accuracy.
What does the middle office do in healthcare RCM?
It converts clinical work into claim-ready accuracy through documentation integrity, coding, charge capture, and record readiness.
Why do middle office problems cause denials?
Because many denials originate from documentation gaps, coding mismatch, or missing charges—issues created before claims are submitted.
What’s the fastest middle office fix?
Enforce documentation-ready and claim-ready gates and standardize handoff packets so downstream teams stop chasing missing information.