Revenue Cycle Management (RCM): What It Is, What It Includes, and How the Cycle Works
What Revenue Cycle Management (RCM) Means in Healthcare
Revenue cycle management (RCM) is the operational system healthcare organizations use to capture, manage, and collect revenue tied to patient care—from the patient’s initial appointment or encounter through the final payment of the balance.
RCM is not a single department and it is not “just billing.” It is the full chain of administrative, clinical, and financial workflows that determine whether care delivered becomes revenue collected.
Operator reality:
Most revenue problems visible in accounts receivable (A/R) were created earlier—during registration, eligibility, documentation, coding, or claim quality checks. When back-end teams are constantly firefighting, the front-end and middle office are usually leaking defects.
Who This Applies To (By Scale)
RCM exists everywhere, but the failure points differ by organization size.
Hospitals / IDNs
- Complex payer contracts
- Multiple departments and handoffs
- Higher denial and underpayment complexity
Large Groups / Multi-Site Clinics
- Standardization challenges
- Training drift across locations
- Denials appear “random” without tracking
Small Practices
- Limited staff and informal controls
- One person’s workflow becomes “the system”
- Errors repeat quickly when unchecked
This guide applies to all three, with scale-specific decision notes where it matters.
The RCM Cycle Steps: From First Encounter to Final Payment
A stable revenue cycle follows a predictable sequence:
1. Scheduling and Registration
- Accurate demographics captured
- Correct insurance captured
- Patient identity and plan details confirmed
2. Eligibility and Financial Clearance
- Eligibility verified
- Prior authorization initiated when required
- Patient responsibility and expectations addressed early
3. Clinical Encounter and Documentation
- Care is delivered
- Documentation supports services rendered
- Medical necessity is clearly supported
4. Coding and Charge Capture
- Charges captured completely and on time
- Codes align with documentation and payer rules
5. Claim Creation and Submission
- Claim built and validated through edits/scrubbers
- Claim submitted (often via clearinghouse workflows)
6. Adjudication and Payment Posting
- Payer processes the claim
- Payments and contractual adjustments posted accurately
7. Denials, Appeals, and Rework
- Denials categorized and corrected
- Appeals submitted when appropriate
- Root causes fed back upstream
8. A/R Follow-Up and Patient Collections
- Unpaid claims followed up on a defined cadence
- Patient statements and self-pay workflows executed
9. Final Balance Resolution
- Balance paid, appealed, adjusted, or written off per policy
Healthy cycle rule:
When controls work, teams prevent rework instead of chasing money.
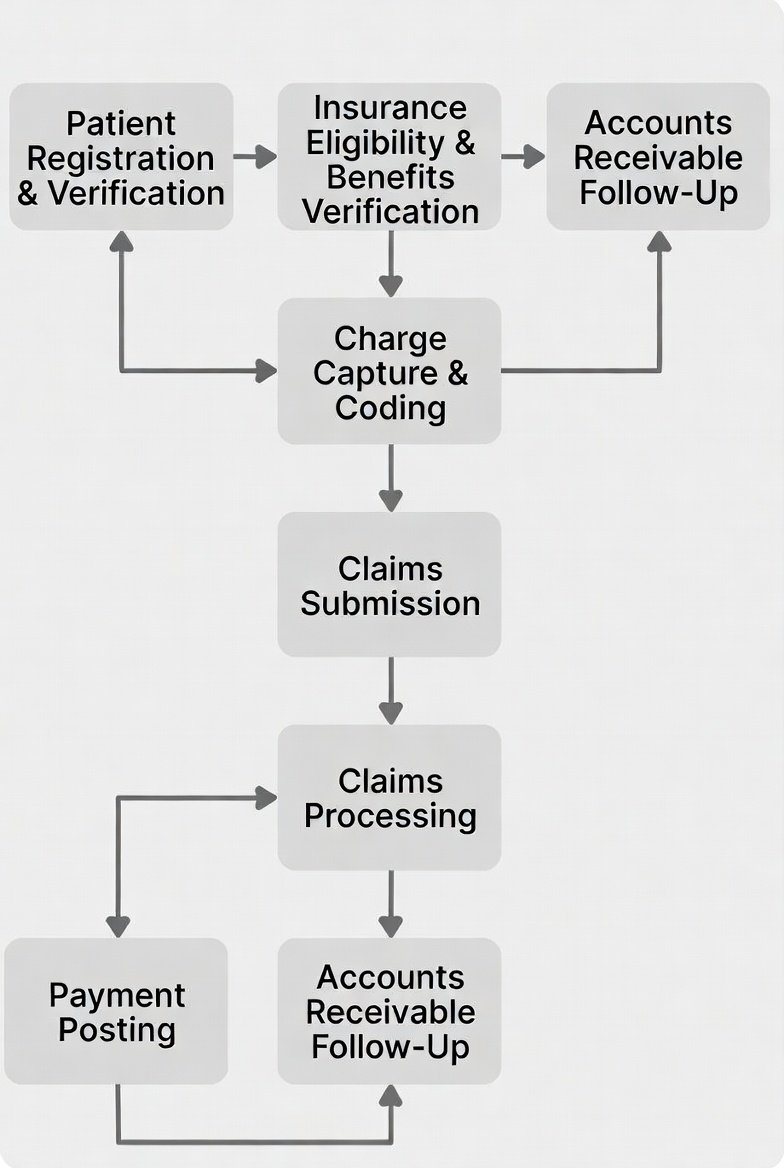
The 3 Parts of RCM
Front-End RCM (Pre-Service / Point-of-Service)
Goal: Prevent avoidable denials and reduce patient-balance surprises.
- Registration accuracy
- Eligibility verification
- Authorization workflows
- Estimates and payment planning
Middle Office RCM (Claim Quality and Revenue Integrity)
Goal: Send clean claims and protect revenue.
- Charge capture completeness
- Coding accuracy
- Claim edits and scrubbing
- Documentation alignment
Back-End RCM (Cash Retrieval)
Goal: Resolve denials and collect what is owed.
- Payment posting accuracy
- Denials and appeals workflows
- A/R aging management
- Patient collections
One-line truth:
Back-end performance is capped by front-end discipline.
RCM vs Medical Billing
Medical Billing Includes:
- Claim submission
- Payment posting
- Denials handling
- Patient billing and collections
RCM Includes:
- All billing functions
- Plus registration, eligibility, authorization
- Documentation integrity
- Charge capture
- Analytics and governance
RCM is the operating system. Billing is one module inside it.
Where Revenue Leaks Actually Start
1. Registration Data Errors
- Incorrect payer or subscriber details
- Outdated plans or demographics
Downstream symptom: Rejections, delays, patient disputes
2. Eligibility Not Verified (or Verified Too Late)
- Missed or inconsistent checks
Downstream symptom: Avoidable denials and patient frustration
3. Authorization Timing Confusion
- Unclear ownership or timing
Key distinction:
- Prior authorization = decision before services
- Pre-claim review = decision before claim submission
Downstream symptom: “Missing auth” denials
4. Charge Capture Gaps
- Missed or late charges
Downstream symptom: Underbilling or late filing risk
5. Dirty Claims Escaping Quality Gates
- Preventable errors submitted
Downstream symptom: Higher cost-to-collect and delayed cash
Ownership Clarity (Stage → Owner → Failure Symptom)
- Registration → Front desk / Patient access → High rejections, demographic mismatches
- Eligibility → Clearance team → Coverage denials, patient disputes
- Authorization → Auth / UR team → Missing-auth denials
- Coding & Charge Capture → Coding team → Underbilling, failed edits
- Claim Submission → Billing → High rejection rate
- Payment Posting → Posting team → Incorrect adjustments
- Denials & Appeals → Denials team → Repeat denial reasons
- A/R Follow-Up → A/R team → Aging balances and cash delays
Key takeaway:
If “everyone owns it,” no one owns it.
When to Fix In-House vs Outsource vs Buy Software
Fix In-House When
- Volume is stable
- Workflows can be standardized
- Issues are discipline-related, not tooling
Best for: Small practices and committed groups
Outsource When
- Staffing gaps or high turnover exist
- Denials and A/R backlogs are heavy
- You want SLA-driven performance
Best for: Small-to-mid groups needing fast stabilization
Buy or Upgrade RCM Software When
- Visibility is lacking
- No shared work queues or denial analytics
- Manual tracking has become a tax
Best for: Large groups and hospitals
Rule of thumb:
If you can’t see your top 10 denial reasons weekly, you don’t have an RCM problem—you have a visibility problem.
KPIs That Show Cycle Health
- Clean claim rate / first-pass yield
- Denial rate and top denial reasons
- Days in A/R
- Aging buckets
- Net collection rate
Start with the KPI tied to your biggest defect, then fix upstream.
RCM Stabilization Checklist (Minimum Controls)
- Eligibility verification is consistent and documented
- Authorization timing and ownership defined
- Charge capture completed within a set window
- Claim edits block known preventable errors
- Denial reasons reviewed weekly
- A/R cadence and aging thresholds enforced
- One accountable owner per stage
FAQs
What breaks first when cash slows down?
Eligibility discipline, charge capture timing, or claim-quality gates usually drift first.
Why do denials feel random?
They aren’t. Repetition means the same upstream defect keeps escaping.
Is prior authorization part of RCM?
Yes. Authorization directly affects whether services are covered and paid.
What is a realistic clean-claim target?
Benchmarks commonly target 95%+ clean-claim performance, adjusted for payer mix.
RCM vs billing—what’s the difference?
Billing executes claims. RCM ensures claims succeed.